Technical Article Of The Day
New in Journal of the American Medical Association (JAMA), a review of the national and state-level impacts of the Affordable Care Act…by Barac...

Senate: 48 Dem | 52 Rep (range: 47-52)
Control: R+2.9% from toss-up
Generic polling: Tie 0.0%
Control: Tie 0.0%
Harris: 265 EV (239-292, R+0.3% from toss-up)
Moneyball states: President NV PA NC


Click any tracker for analytics and data
I’m fortunate to work at an institution that requires full vaccination, including boosters. Princeton University also is fairly aggressive on safety measures for in-person teaching. With Omicron on the rise, is it enough?
On this topic. I recently corresponded with my colleague Eve Aschheim, an in-person studio art instructor. She asked if current precautions were enough. I thought yes – especially if students wear KN95 masks in class and there was a portable HEPA filter running. I also came up with a simple “multiply/divide by 3” rule to allow for Omicron.
Our conversation follows, lightly edited.
Eve Aschheim: I’m curious as to your thoughts on Omicron, and how one might avoid transmission in the classroom.
My class, a studio art class, is 4 hours…and we are in close proximity, 12 or so students in a slightly larger than standard classroom, perhaps 18’ x 25’. While the University seems to have done a great job in avoiding infection clusters in academic settings in the past, Omicron changes the dynamic with its greater infectiousness, and I am unaware of any extra measures the University has recommended for classrooms in the current situation.
I’m sure you have seen this chart circulating from The Wall St. Journal on previous mask guidance. Last semester I wore an N95 for 4 hours with most students wearing cloth masks (despite my pleas to wear the KN95 and N95 I provided), so it appears from the chart that both I and they were at risk for contracting the virus, so it was probably just luck and low numbers of infections that protected us.
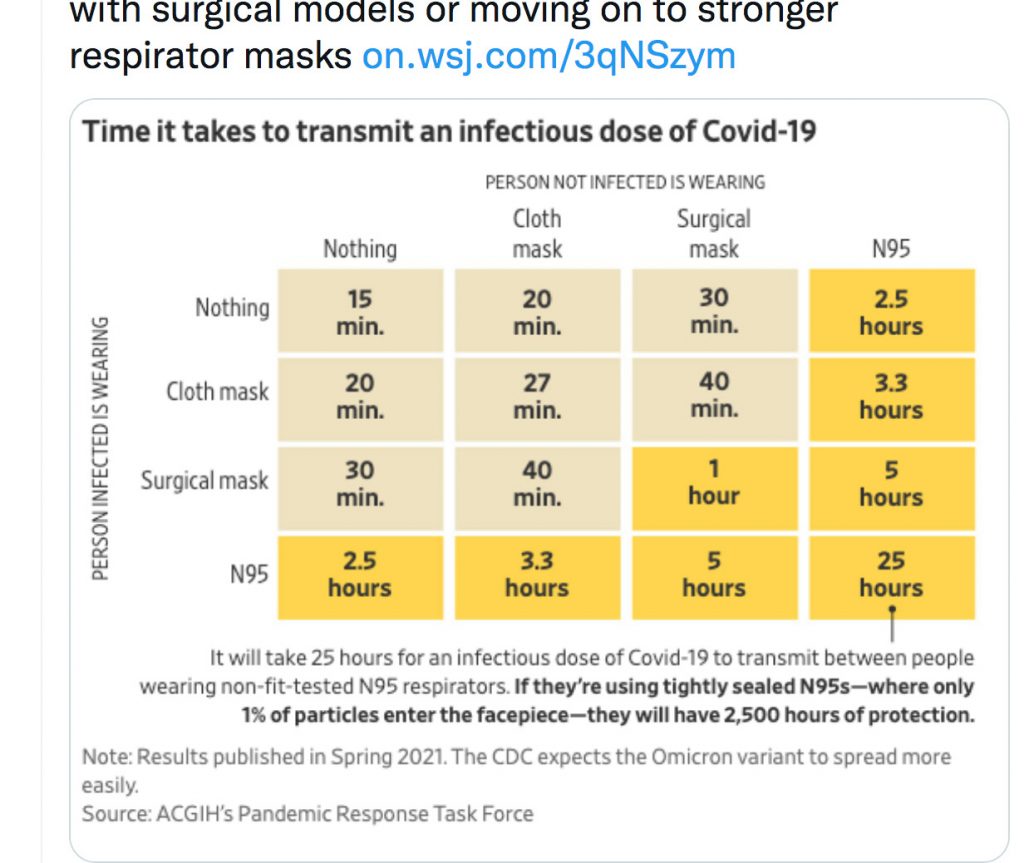
Sam Wang: First, don’t forget that this WSJ chart assumes that people have a good fit on their masks – no nostrils showing or mask-edge leak allowed! Also note that KN95 masks become somewhat less effective after 40 minutes or so on account of moisture, so it’s good to have a spare you can switch to. (They can be dried out again.)
In regard to whether you got lucky, the near-universal vaccination in our community works in our favor. I taught two classes in the fall, each with fewer than 10 students. I did some calculating based on a per-week infection rate of 0.1%. and estimated about a 1 in 4 chance that someone covid-positive was in the class at some point in the semester. In that circumstance, masking reduces the risk of transmission enough to make it safe to meet.
One precaution you may wish to take is to get a HEPA filter. I routinely use one in my classes. In a room the size of your class, this Coway filter would achieve 99.99% clearance of particles smaller than 5 microns in 15 minutes.
I agree that Omicron increases the transmission risk substantially. Omicron hit New York City in early December and then started spreading toward Princeton. Our classes missed out on Omicron…but now we have time to prepare by spring.
Perhaps we should push for the deployment of portable HEPA units throughout the laboratory and studio spaces on campus. I would gladly join you in making such an approach.
Eve: This info on KN95 is very useful, and I did not know it.
I have a BlueAir filter 211+ running in the class and I stand by it at times, though I run around a lot. I remember you suggested this in your twitter post, and I actually had it running prior to Covid for the immense dust. Do you think that is adequate for our room? I also try to open a window, weather permitting.
I like your calculations on class exposure risk. My class runs 4 hours, and yours might be less, right? Can we update the stats with the Omicron variant?
The students seem very lax about mask quality and other precaution factors, so their risk of infection is much greater than mine, but I still would prefer they not get sick!
Please let me know if you learn anything new re transmissibility.
Sam: I looked up the specifications on your filter. It is rated to change the air in a 540 square-foot room five times per hour. Your room is smaller than that, so that means all the air in the room goes through that filter every 12 minutes, tops. I think that is good protection. I would characterize it as similar to the effects of putting a KN95 mask on everyone who isn’t wearing one.
For maximal effectiveness, a HEPA filter should be placed nearest to the largest source of aerosolized particles. In the case of a class, that would be the instructor, who is speaking the most. Opening the window is also good practice.
The students spend a lot of time in proximity with one another outside class. During the term I had dinner with one of my students over at Whitman College. On another occasion, I went to dinner in Forbes College, where I am a fellow. While they’re eating they are unmasked. So class time is only a small part of their risk. But the masking is certainly important to protect us.
You are correct that the WSJ table you saw should be corrected to account for Omicron. It is hard to do that precisely, but I would divide all the numbers by 3 for starters.
Eve: May I quote you regarding the chart? “Sam Wang says to divide all the numbers by 3 for Omicron”? People are dying to know what the standard is!
Sam: (panics, starts to download a ton of literature)
It’s just an estimate off the top of my head! I suppose you could say you heard it from me at what passes for a party these days, which is email.
Now you have sent me down an enjoyable (to me) rabbit hole of estimating this particular number…
Eve: This is an important rabbit hole!
Two hours later…
Sam: Turns out I made a lucky guess. A fair bit of evidence points toward a factor of 3.
I found two calculations based on various assumptions. One (Sofonea et al.) suggests Omicron spreads 2.4x as fast as Delta. The other (Nishiura et al.) suggests a factor of 3.3-4.2x. Averaging these two gives about a factor of 3 for increased transmissibility.
The viral load in an infected person might be about 4 times larger for Omicron compared with Delta. One press release claimed it was a factor of 70, which was eye-grabbing. However, a closer look at that study shows that at 48 hours, probably the most relevant time point (see my tweetstorm), the difference was more like a factor of 3. However, that study also says that Omicron grows about 24 hours earlier than Delta. This helps account for the explosive spread of Omicron.
Anyway, the big takeaway for classroom teaching is that an Omicron-infected individual might typically shed 3 times as much virus than a Delta-infected person.
When it comes to time, like the times in that Wall Street Journal chart, divide by 3 to get an accurate estimate on safe exposure times. Also, adding a HEPA filter will add a layer of protection that could be quite useful – it probably equals (in the opposite direction) the effect of Omicron, more or less.
When it comes to people, multiply by 3. See five people in the store? Imagine 15 people. Wow!
When it comes to distance, increase by 50% (there’s some math involving cube roots, don’t worry about it). So instead of 6 feet, keep to 9 feet.
Rutgers is fully online until end of January. I am moving all my material to Canvas, but I wonder what instructors in visual and performing arts, laboratory courses etc. are going to do.
Studio arts courses have been dealing with this question since the beginning (March 2020 for me). The answer is – it’s hard. We are doing what we can – but teaching studio courses online is definitely an added level of difficulty compared to a more “standard” lecture type course.
Hey Sam, do you have a source on the KN95 moisture issue reducing their effectiveness after 40 minutes?
See
https://www.espublisher.com/uploads/article_pdf/es8d1110.pdf
Be aware of moisture’s effect on mask life
The Nursing Times makes the point that:
A mask wet with exhaled moisture has increased resistance to airflow, is less efficient at filtering bacteria and has increased venting. Current recommendations are that a new surgical mask is used for each surgical case and that they should be changed when wet.
This point is echoed by the WHO as well, therefore, if a mask has become wet (or soiled, of course), it should be disposed of regardless of the length of time that it has been worn.
The problem with wearing N95 respirators for extended periods
N95 respirators filter the air that the wearer breathes, removing airborne particulates, such as virus particles, and protecting the user. The need to breathe through the materials puts a strain on the user, and so while extended use may be possible, it is not easy or recommended:
When worn properly, these respirator masks get very hot inside and are very difficult to breathe in due to the pressure change between the air inside and the outside atmosphere. It is like breathing through a blanket and can become distressing to the user. A user’s blood-oxygen saturation can drop and carbon dioxide increases significantly with correct and prolonged use. Even a healthy and fit adult could find wearing an N95, if put on correctly, difficult after an hour or so of use. An older person or an immunocompromised individual likely would have a very hard time using an N95 mask even for a short time. Wearers may take it off for a break which would reduce its protection. Children and infants are also generally not appropriate candidates for wearing N95s as the risk of suffocation is higher.
Hi Sam, thanks for this. Two questions:
– What proximity and activity do the WSJ chart, and your modifications, assume about the two people? Are they standing within six feet and talking to each other, for instance?
– Wouldn’t an air filter need to filter air at least as fast as air is cycled through a person’s lungs, and so for a room with more than one person, the rate required would scale upwards with each additional person? And then it may need to be adjusted for the particular activity (listening to a lecture vs classroom discussion, for example.) I’ve been looking for guidance about this, since it seems obvious, but I’ve had no luck.
Thank you so much!